As I’m sure we’ve more than adequately demonstrated, transdermal delivery is not only a more efficient and effective way to transport nutrients from outside to within, but in a society plagued with digestive disorders, it may be the only means (besides intravenous) of correcting deficiencies or benefiting from a prescribed treatment. However, the skin is still by far one of the most under-utilized vehicles for drug delivery when it comes to mainstream medicine… or even alternative medicine for that matter. Only in recent years have people started taking more notice (Patches! Patches are everywhere!).
So… given my penchant for reading any and all magnesium-related research, it’s not surprising that a recently released article caught my eye and inspired this post. Interestingly enough, the article actually discussed the absorption of magnesium transdermally, which I was very excited about. But even more interesting (to me, at least) was that the transdermal application came with a dose of electricity.
Iontophoresis
For those of you who are unfamiliar with iontophoresis, also known as electromotive drug administration (EMDA), this is a completely non-invasive, topical treatment that somewhat resembles electrical muscle stimulation (EMS). Unlike a muscle stimulator, however, an iontophoresis machine uses a repulsive electrical current to move the chosen drug – or, in the case of this research study, magnesium – across the skin barrier. 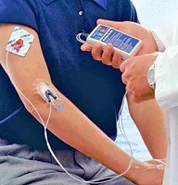
In this 2013 study, Electromotive Drug Administration of Magnesium Sulphate on Spastic Biceps Brachii of Stroke Survivors, iontophoresis and cryotherapy (a.k.a icing) were both utilized in the application of a magnesium sulfate gel on stroke survivors who were experiencing muscle spasticity. Despite the relatively infrequent & brief usage of the treatment, which was detailed as being “repeated twice a week for 4 weeks,” both the iontophoresis group as well as the cryotherapy group showed a significant reduction in spasticity.
During the discussion portion of the article, the method of transdermal drug delivery and its uses was detailed further:
Transdermal drug delivery has numerous advantages over traditional oral and intravenous delivery routes because there is avoidance of risks and inconveniences usually associated with the later. The liver is bypassed in terms of first pass elimination and both local and systemic treatment effects are derived.”
Although this isn’t a new or profound insight, and transdermal delivery has been making more frequent appearances in recent research studies, the clinical analysis of its uses in conjunction to mineral therapies is a both welcome as well as reinforcing. Even better, they went on to articulate the benefits of magnesium:
Magnesium affects peripheral nerve by interfering with the release of neurotransmitter substances at synaptic junctions or potentiates the action of local anaesthesia. It has been noted not to be toxic when administered through skin and it does not also vaporize easily.
Magnesium sulphate blocks peripheral neuromuscular transmissions by reducing acetylcholine release at the myoneural junction, resulting in inhibition of skeletal muscle contraction. Magnesium is a cofactor for enzymatic reactions which plays important role in neurochemical transmission and muscular excitability and the ions elevate the firing threshold in both myelinated and unmyelinated axons.”
In other words, magnesium is able to regulate transmissions to both nerves and muscles, mediating abnormal or excessive activity such as spasms, cramps, and twitches. Applied using iontophoresis, the magnesium readily permeated the affected area and was able to immediately benefit the patient. Cryotherapy did, of course, show a decrease in spasticity as well, but not to the extent of the iontophoresis. This treatment, repeated over time, was shown to be more efficient, produce more significant results, and ultimately be more cost effective than other clinical therapies.
The downside? Getting your hands on a personal iontophoresis machine can be a bit costly. However, there are more and more physicians and physical therapists that are integrating these into their practices. Up until now, iontophoresis has been more commonly applied to people suffering from hyperhidrosis in their hands and feet, but as we can see, other uses are being explored.
——-
For those of you who are technically inclined or curious, there are nooks and crannies of the vast internet that detail how iontophoresis works and the tools needed to create your own. That is not a recommendation to do so, but it certainly never hurts to have a better understanding of just what this application entails.
If you want to know more about transdermal delivery, we have additional information on how topical magnesium works.
Or, if you have any questions regarding this article and iontophoresis, please feel free to comment or email us directly.
